Survey reveals how states are implementing Medicaid work requirements
By Jennifer Pallikkathayil / May 13, 2026
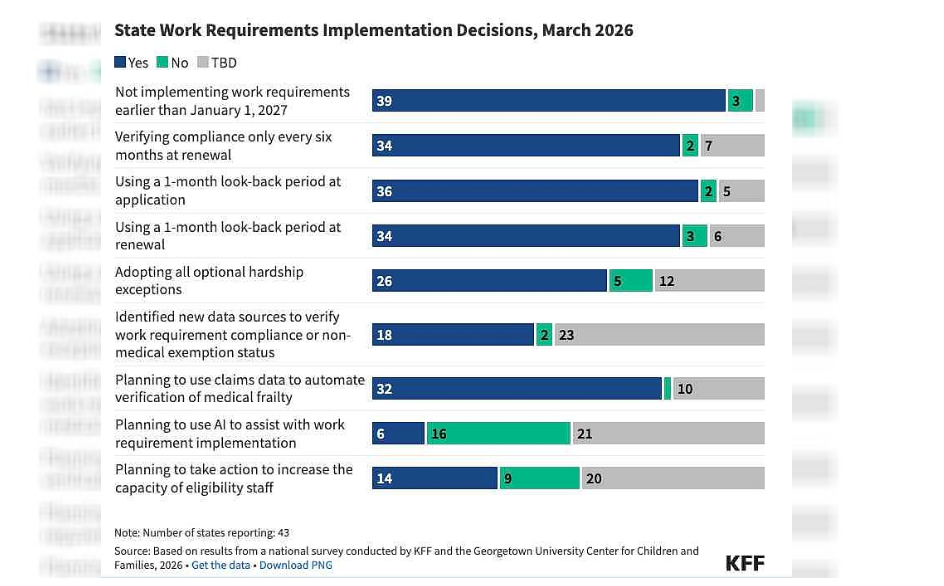
A new KFF survey found that states are taking varied approaches to implementing Medicaid work requirements.
The survey studied responses from state Medicaid officials and focus groups in eight states -- Arizona, Indiana, Montana, Nebraska, Ohio, Pennsylvania, Virginia and Washington -- to learn more about how states are handling the new implementation requirements.
The survey found that, of the eight states, seven are planning either stricter verification of work or exemption status or earlier implementation of the requirements, according to the alert. The plans are slowly emerging as states report facing constraints with time, costs and other issues -- including how to define and verify certain exemptions because of delayed guidance from federal authorities.
The 2025 reconciliation law, also known as the One Big Beautiful Bill, requires that adults in 43 states (and Washington, D.C.) covered through the Affordable Care Act Medicaid expansion and partial expansion waiver programs meet work requirements starting Jan. 1, 2027.
According to KFF.org data, Missouri plans to implement the verification process Jan. 1, 2027, and individuals will be required to have 80 hours a month of work or qualifying activities. About 60 percent of Missouri's Medicaid adults who don't have dependent children, and who could be subject to work requirements, reported working at least 80 hours per month or attending school, according to KFF data from 2024.
In the report, 29 states -- including Missouri -- plan to adopt a hardship exception for those facing "extenuating circumstances, including exemptions for individuals who live in high-unemployment areas or areas experiencing a natural disaster, individuals receiving care in a hospital or nursing facility, and those who must travel for medical care," according to the news brief.
In addition to implementation decisions and planning, states are having to face other challenges and uncertainty, according to the news brief. One major issue it cites is resource constraints. This means in order to reduce burdens on Medicaid enrolles and administrators, states are being required to use available and reliable data sources to verify compliance with or exemptions from work requirements.
However, according to the news alert, states say their efforts to automate verification processes using new data are limited by time, costs, staff capacity and other operational challenges.
States are also reportedly awaiting federal guidance on how certain exemptions and community engagement activities should be defined, as well as what verification methods are accepted. For example, states want more information on who qualifies as "medically frail," who qualifies as a caregiver and how caregiver should be defined, according to the news release.
According to the news alert, six states -- including Missouri -- are planning to use artificial intelligence to help implement work requirements.